The current coronavirus situation raises questions in a whole range of areas – such as hygiene and handling respiratory therapy equipment. We will show you what you need to watch out for.

Inhalation and other respiratory therapy measures are day-to-day routine for most people with chronic respiratory disease. Some patients with acute respiratory infections or COVID-19 have to use inhalation therapy. This reduces respiratory symptoms, such as shortness of breath.
Inhalers, nebulisers, holding chambers, PEP systems and devices that measure lung function are used in these cases – at home, at the physiotherapist, at the doctor’s practice and in the hospital. This raises the question of how safe it is to use respiratory therapy equipment during the coronavirus outbreak? What hygiene guidelines should be applied to COVID-19 patients? Has anything changed in terms of using the equipment at home?
We give you an overview of what you have to consider when using, cleaning and disinfecting inhalation devices and other respiratory therapy equipment during the coronavirus pandemic.

Independent laboratories have deemed the measures for hygienic re-use of PARI medical devices, as recommended in the current instructions for use, to be safe and efficient. They also provide the level of safety needed at the moment. The thermal disinfection and sterilisation methods inactivate heat-sensitive viruses. For this reason, you do not need to change the way you are cleaning and disinfecting your inhalers and your other respiratory therapy equipment.
If components cannot be disinfected by boiling or vaporising, wipe with chemical disinfectant classified as “limited virucidal activity” or “virucidal”. This offers the necessary safety for virus inactivation.
As a further safety precaution, and one which is generally recommended for patients at risk, you should not share medical devices with other people at home. Every patient should use their own device (“single patient use” mode). This also applies to COVID-19 patients.
The use of disinfectants is being encouraged due to coronavirus. However, extensive use of disinfectants can have its drawbacks. The risk of accidental poisoning rises. Skin diseases are more likely to develop and there is also the risk of pathogen resistance. This is why it is important to avoid chemical disinfectants wherever possible.
Respiratory therapy equipment from PARI is designed so that all non-electric parts such as nebulisers, aerosol generators, filter/valve sets, PEP systems, spacers, and so on can be thermally disinfected. Boiling and vaporising are validated methods of disinfection. They are efficient, safe and do not require any chemicals or alcohol.
The general cleaning and disinfection recommendations for PARI medical devices are still safe and efficient during this coronavirus pandemic, be it at home, in the physiotherapy or doctor’s practice or in the hospital.
A range of different respiratory therapy equipment is used for coronavirus patients. We will show you what you have to consider for the hygienic preparation of the various inhalers and devices at home.
Nasal rinses have long been recommended for the prevention and therapy of viral colds or pollen allergy. Nasal rinses work by mechanically cleaning and flushing the mucous membranes inside the nose. Secretions, dried mucus and pathogenic intruders such as pollen and germs (viruses or bacteria) can be flushed out. Nasal rinses can therefore be seen as a very simple and potentially helpful measure. After all, viruses that have been flushed out of the nose cannot do any more harm. Generally speaking, a nasal shower should always only be used by one person. Even within a family, every member should have their own nasal shower.
After use, disassemble the nasal shower and clean with warm water. Once a day you should boil or vaporise the dismantled nasal shower, as described in the instructions for use. This procedure also applies if you use the nasal shower during a coronavirus infection.


Inhalers such as the PARI BOY consist of several components:
If you are inhaling at home with a nebuliser due to having COVID-19, please use the nebuliser in “single patient use mode”, i.e. only you and nobody else, not even another member of your family, should use the same nebuliser as you. This “single patient use mode” is always recommended for high risk patients.
For hygienic preparation at home proceed as set out in the instructions for use for your PARI BOY:
Remember that the nebuliser generally has to be replaced after one year. All accessories are supplied together in the PARI Year Pack.
After you have finished the inhalation therapy, remove the nebuliser. Leave the tubing connected to the compressor and allow the compressor to run for a few minutes. If the tubing has become damp on the inside, this will allow it to dry. If liquid enters the tubing during inhalation, rinse with warm water and connect to the device without the nebuliser. Run the compressor until the tubing is dry.
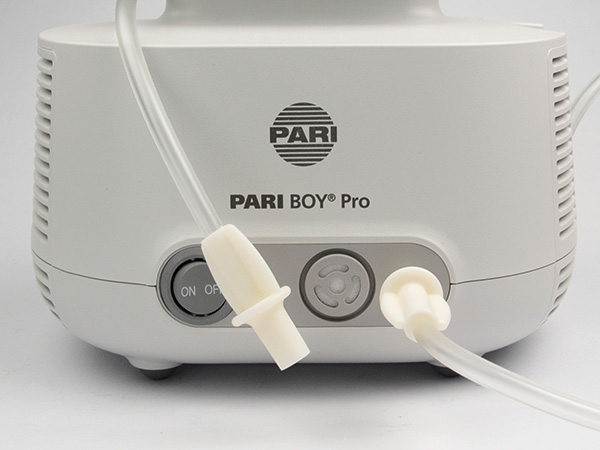
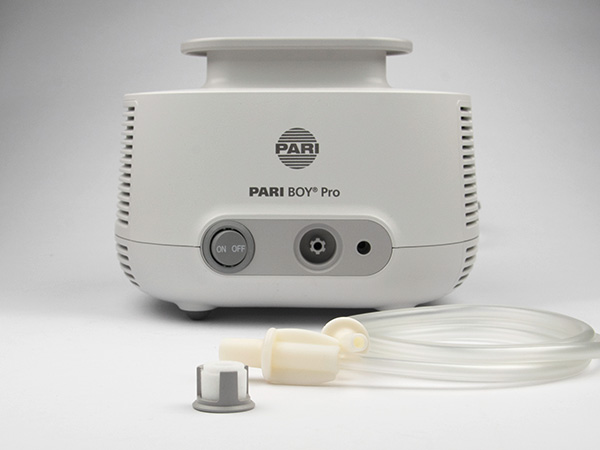
Wipe the compressor with a damp cloth after every inhalation. Once you have recovered from COVID-19, wipe the device with disinfectant. Then store the compressor in isolation for 9 days – for example in a closed box. You should also change the compressor filter.
Tip for use at home: Once you have recovered from COVID-19, replace the connection tubing and filter. Both are available in the PARI Year Pack along with a new nebuliser.
If patients have to inhale metered aerosols (sprays), this can have certain disadvantages, irrespective of the diagnosis: coordination problems in patients (simultaneous pressing the trigger and inhaling), a relatively high deposition rate of particles in the mouth and throat and a possible cold stimulus in the patient’s throat are familiar drawbacks of this form of therapy. The use of a spacer overcomes these obstacles. In the case of infectious diseases, it is important that these medical devices can be prepared so that the meet high patient welfare standards.

The VORTEX holding chamber should be used at home in “single use mode”, i.e. only one person may use the holding chamber.
For the hygienic preparation of the holding chamber, proceed as set out in the VORTEX instructions for use.