The coronavirus pandemic means that wearing a face mask is the order of the day. But in practice, the piece of cloth does raise questions. This article will address FAQs posed by patients with lung disease.

Wearing a face mask is now de rigueur in Germany. But this goes hand in hand with a wide range of problems and questions on their use. As high-risk patients, anyone with chronic respiratory disease has to be especially careful to protect themselves from coronavirus. The Robert Koch Institute reported in its status report at the beginning of May that “the risk to the health of the population in Germany is currently estimated to be generally high, and very high for risk groups”.
Proper and hygienic handling of masks, in particular, is therefore extremely important for lung patients in Germany in each and every situation.
Can I cough into the mask? Is it normal to have problems breathing with the mask on? What happens if I am short of breath or have an asthma attack with the mask on? What happens if I have to take off my face mask for a pulmonary function test? What are associations and clubs in Germany telling their members about the obligation to wear a mask? We have collected the most frequently asked questions from patients with lung disease, have looked into the answers and compiled them – because we are sure that some of the questions will be interesting for people living abroad too:

No, patients with lung disease are not basically exempt from having to wear a mask. Exemption from mandatory masks is only granted in Germany if wearing a face mask would pose a serious risk to health or is impossible for medical reasons. In these cases, however, out of consideration for other people, it makes sense to avoid public transport and shops wherever possible.
In Germany, it is also possible to have a doctor's certificate stating that it is unreasonable for you to wear a mask and to take this with you in case there is an inspection. The exemption applies in all states in Germany aside from Saxony-Anhalt, as can be seen in an overview provided by the German Respiratory Health League. There is no official exemption in Saxony-Anhalt. The German Respiratory Health League also points out in a PDF publication on the obligation to wear a mask that issuing what has been dubbed an “unreasonableness certificate” is not a service covered by the health insurance and may be subject to a fee. If you would like a certificate you can call or write to your doctor to enquire about this. However, the decision as to whether a certificate is issued is at the discretion of your doctor.
Breathing through a face mask takes some getting used to and is more difficult for anyone than without a mask. Anything that covers your mouth and nose is a barrier. This barrier varies in strength depending on the filter performance, whether the mask has a valve or not (for FFP masks) or the type of material it is made of in the case of face masks.
Breathing through a very close fitting and dense face covering made of several layers of fabric can be an enormous strain for people with chronic lung disease in particular, according to the Robert Koch Institute spokesperson and the mask manufacturer 3M in answer to a question raised by the research network Correctiv.
It is normal for this to be an unpleasant sensation. But if you start to feel ill when wearing a mask, this can be a warning sign. Edwin Bölke, senior physician at the Clinic for Radiotherapy and Radiooncology of the University Hospital Düsseldorf writes in the medical journal Ärzteblatt that headache, dizziness, a rash or muscle twitching, for example, could be warning signs of hypercapnia (condition of abnormally elevated carbon dioxide (CO2) levels in the blood). He goes on to say that people with chronic respiratory disease are at risk of developing hypercapnia in response to intense physical exertion. This means that if carbon dioxide (CO2) is not properly expelled because of the high air resistance in the mask, it could accumulate in the blood. Increased levels of CO2 in the blood can have an additional detrimental impact on health.
The German Respiratory Health League points out that in practice, those affected will automatically take off the mask in time. They also point out that harmful increases of pCO2 by masks have not been proven. Wearing a surgical mask or a homemade mask is harmless, according to the German Respiratory Health League because these masks “.... leak significantly and an increase in pCO2 is therefore very unlikely. However, patients may feel that covering their nose and mouth is unpleasant or threatening or may subjectively feel that they are short of breath. Breathing in the moist air can also be unpleasant.”
The DAAB, the German Allergy and Asthma Association, also does not see wearing simple masks as critical but does point out that “Patients with respiratory disease who want to use FFP2 or FFP3 masks for their own protection should definitely discuss this with their GP and/or pneumologist. Generally, we do recommend that high-risk patients avoid contact with others as much as possible and, given the persistent risk of infection, that they religiously follow the hygiene advice.”
Tip: Try out different masks at home to find out which you can handle best.
In Germany, if you have acute breathlessness, a panic attack or an asthma attack you may take off your mask. If possible, leave the shop or public transport. Then do as you usually would. For example, take the asthma spray your doctor has prescribed. If necessary, inform a doctor. In these situations, you should also try to handle your mask properly and try to stay calm.
Yes, you may. Remember to cough or sneeze into your elbow, even if you are wearing a mask. This ensures the force of air does not propel the virus into the atmosphere, which could then end up on the outside of your mask. If the inside of your mask has secretions on it and is very moist, change your mask. The moisture means that the mask loses its protective function.
No, nothing changes here. Put the face mask on and take it off just as you would without the oxygen therapy glasses. But the lung specialist, Prof. Dr Rainald Fischer, does point out that “the face mask cannot fit tightly because of the oxygen tube that goes over the cheek. This means that a small amount of air you exhale will enter the environment. If the patient is wearing an FFP2 or FFP3 mask, this no longer offers 100% protection as air from the outside can enter the gap.”

In Germany, you have to take off the mask for a pulmonary function test. For X-rays, anything made of metal generally has to be taken off, so that includes masks with a metal strip. Take your mask off properly. Disinfect your hands first, then take off your mask. Only touch your mask by the straps and elastic. You can store the mask in a container in the meantime.
Place the mask with the outside face down in a clean container you have brought from home. There are two reasons for this: Firstly, the outside of the mask does not touch any potentially contaminated surface. And secondly, any germs on the outside of your mask are not transfered to the surface. The container you briefly put the mask in has to stay open and inaccessible for other people. During the X-ray, the mask and container remain in the changing room. For the pulmonary function test, you can, for instance, take the mask into the lung function cubicle with you and hold it on your lap. Before you put the mask on again after the test, remember to disinfect your hands.
Alternatively, you can temporarily store the mask and put a new one on after every examination. But this does mean that you will need three masks if you have a lung function test and an X-ray examination on the same day.
No, you should not do that. You see people doing this a lot, but they shouldn’t. You cannot tuck your mask under your chin, push it up into your hair or even just wear it on one ear or hang it onto the outside of your bag. Doing this can allow germs that are on your skin, hair, clothing or bag to reach the inside of the mask and contaminate it.
This is why, if you want to blow your nose, eat or catch your breath you have to take off the mask the correct way and store it in a container until you put it back on. Before putting the mask back on, remember to clean your hands.
Briefly pushing your mask under your nose is also a bad idea. This rubs virus that may be on the edge of the mask directly under or even into your nose.
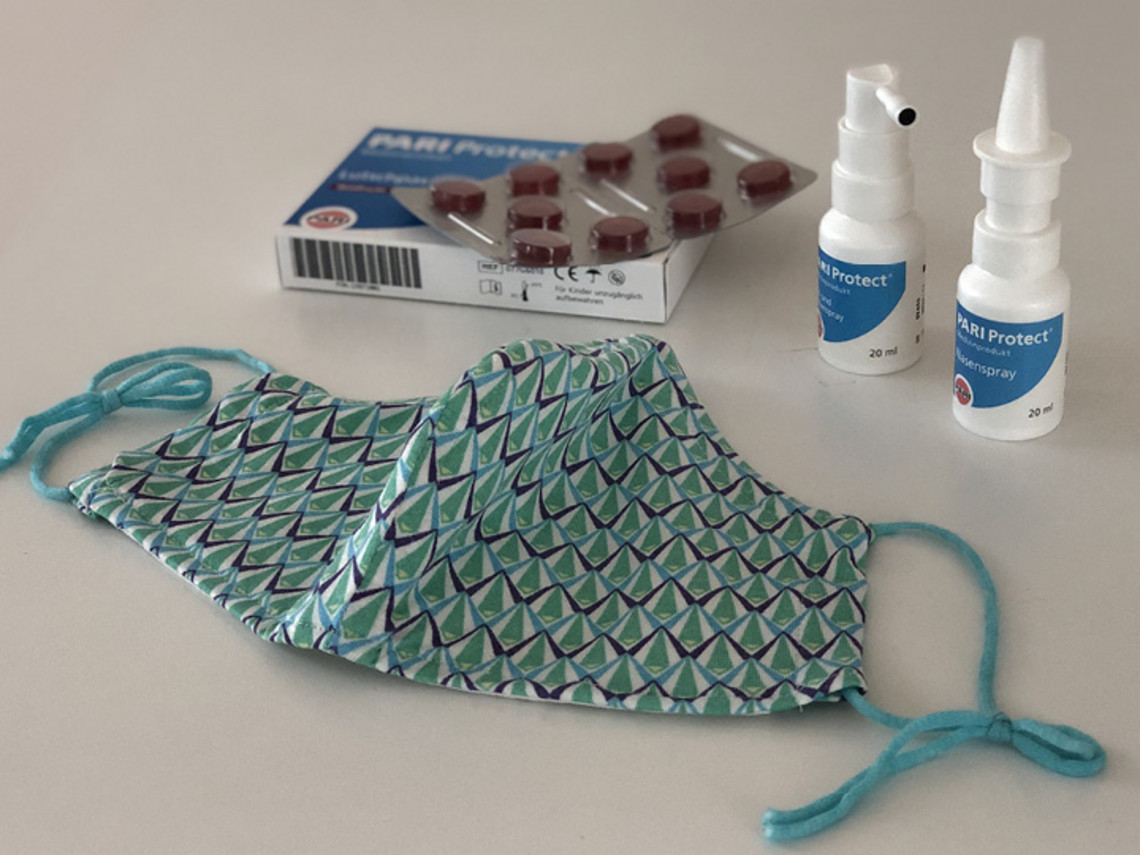
If you wear your mask for long periods, it can dry out your mucous membranes. As this makes them more susceptible to viruses, you should counteract this effect. Make sure you drink enough. You can also moisturise your mucous membranes with nasal spray, throat spray and lozenges containing ectoine or use a nasal ointment.
Washing your hands carefully or disinfecting them before putting on or taking off the mask ensures that no germs are transfered from your hands to the mask or vice versa. When putting on and taking off the mask, your hands are near your head and face. This is why your hands should be as free from dirt or virus as possible.
As a rule, you should touch your face mask as little as possible and make sure that it fits perfectly the first time you put it on with clean hands. If the face mask still slips, you can adjust it to the correct position. It is important that you only touch the edge of the mask. But here, it is still important to remember to disinfect your hands with a hand sanitiser before and after touching the mask. There could be germs on your hands or on the outside of the mask.
If your glasses steam up when you are wearing the face mask, it is not tight enough. The warm and moist air you breath out is escaping upwards through the small gap and meeting the cooler air on your glasses. This makes your glasses steam up. Ensure that the mask fits tightly over your nose and cheekbones. This is best achieved with a face mask with metal nose strips. The face mask may not cover your glasses, by the way.
Always follow the same procedure, regardless of when, how often and at what intervals you use your face mask. This is a step-by-step guide to putting on your mask:
It is important to follow this procedure to keep the inside and outside of the face mask free from viruses or other contamination. Viruses on the inside of the mask can reach your face or the susceptible mucous membranes of your nose and mouth. Viruses on the outside of the mask could be propelled from the outside of your mask into the environment by the force of air when you cough or sneeze.
Change your mask if it is obviously dirty, contaminated or damp. Generally speaking, regardless of the material it is made of, a mask will be moist after wearing it for three to four hours.
The German Allergy and Asthma Association is in favour of wearing a face mask to protect the population against infection with coronavirus, and does not see any problem in most people wearing simple masks made of fabric. This also applies to most patients with asthma or chronic lung disease.
In an info-flyer on COVID-19, the German Respiratory Health League recommends that COPD patients should continue to carefully observe the hygiene rules, should social distance, avoid potential sources of infection and only visit the pneumology practice if it is urgent. They should also continue with their prescribed therapy.
The Cystic Fibrosis Association (Mukoviszidose e.V.) in a statement issued on 5 May 2020, addresses the PARI blog: “Face masks (also known as non-medical face masks), which now have to be worn out shopping and on public transport, serve more to protect others than the individual by preventing the wearer from propelling potentially infectious droplets into the environment when coughing or sneezing. This reduces the risk of transmitting coronavirus and slows down community spread of COVID-19. Only FFP3 masks will offer wearers themselves reliable protection from coronavirus, but aside from the fact that they are difficult to get hold of at the moment, it can be difficult for patients with cystic fibrosis to breathe in one of these masks. Our most important advice for patients with cystic fibrosis, aside from wearing a simple face mask in public, remains: keep social distancing and carefully follow the hygiene advice.”
The Kartagener Syndrome and Primary Ciliary Dyskinesia Association (Kartagener Syndrom und Primäre Ciliäre Dyskinesie e. V.) responded to our request as follows: “We essentially advocate wearing a face mask, as it means that people are being considerate and are protecting each other from infection. This means that people who have primary ciliary dyskinesia, who are in a risk group, are also automatically better protected. Many of our members (especially those severely affected) have been self-isolating as much as possible since the outbreak of the pandemic. As this cannot go on indefinitely, they depend on the solidarity of society at large and on everyone wearing a face mask. People with primary ciliary dyskinesia often have problems breathing through their nose or difficulty breathing in general. Wearing a face mask can make symptoms worse. This is why we believe that exemption rules for wearing a face mask are important.”
Note: The content of this article is not an official recommendation but rather an aid for handling face masks in everyday life. The article was written in early May 2020 and is based on information and recommendations available at this time.