
German Society for Pneumology
The novel coronavirus keeps throwing the world curve balls, raising many questions, including the issue of the treatment of chronic respiratory diseases. One thing we do know is that: according to a NICE statement, also during the coronavirus pandemic, nebuliser therapy is a safe option [2], ensuring your patients receive a reliable and effective therapy irrespective of their age and medical condition [3].
Transmission via small bioaerosols exhaled from the lungs is now widely recognised as an important route of transmission. [4] It is important to differentiate bioaerosols – released by the patient – and medical aerosol generated by a nebuliser. As in the ISAM COVID-19 guidance paper is stated: “Medical aerosols from nebulization derive from a nonpatient source (the fluid in the nebulizer chamber) and have not been shown to carry patient-derived viral particles. Concerns of medical aerosol becoming contaminated in the lungs before exhalation are not supported by evidence. Consequently, when a droplet in the aerosol coalesces with a contaminated mucous membrane, it will cease to be airborne and, therefore, will no longer be part of an aerosol. In fact, aerosol administration has been reported to reduce generation of bioaerosols. [5,6]
Dr. Thomas Voshaar; aerosol expert and medical advisor to the German Ministry of Health


More than a year after the first corona case became known, more and more patients with long-term consequences of the COVID-19 infection are presenting to doctors' practices. Long Covid seems to occur regardless of the severity of the course of the disease. What can one advise these patients to do?
Machado and co-workers from Brazil recently published robust biological data on the possible role of hypertonic saline solution (HS) as a prophylactic and alternative therapy option for COVID-19 in a preprint report. On the basis of their in vitro experiments in epithelial cells of monkeys (Vero cells), they were able to prove that 1.5% NaCl solution can completely block the SARS-CoV-2 replication. They assume that it is an intracellular mechanism of action and that the inhibiting effect of HS on the life cycle of the virus is due to the depolarization of the plasma membrane [8].
These results can be put in connection with earlier in vitro data, which certify hypertonic saline solution in addition to the secretolytic, also anti-inflammatory and anti-infectious effects [9].
In RSV infections of the upper respiratory tract it has already been clinically shown that nasal rinsing and gargling with HS (2-3%) shortens the duration of the infection and can reduce OTC medication, the transmission between people in a household and virus shedding [10]. Currently, two clinical studies with HS as a nasal rinse are also being carried out for COVID-19 [11, 12] in order to prove the effectiveness of HS against SARS-CoV2 in vivo as well.
Due to Machado HS could lead to simple, safe and low-cost interventions at various stages of COVID-19 treatment, improving the prognosis of infected patients, thereby mitigating the social and economic costs of the pandemic.

If budesonide can be recommended in the treatment of COVID-19 is currently discussed controversially. On the following page you will find an overview of the current study situation and when it can be a good alternative to administer budesonide as a nebuliser solution.
Köhler 2007 - formerly president of the German Society for Pneumology (2005-2007)
Find out more about how inhalation with isotonic saline solutions can help keep viral infections at bay. Inhalation with saline solution is generally effective, irrespective of the type of disease pathogen.
PARI nebulisers can easily be sterilised in boiling water, leaving them hygienically safe, without the need for chemical disinfectants.

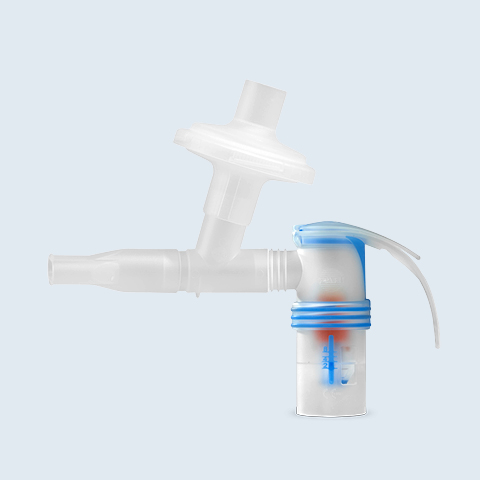
Due to the still existing uncertainty regarding the coronavirus, the use of a filter valve set is recommended in some situations. For example, when COVID-19 patients with chronic respiratory diseases inhale with a nebuliser in the hospital.
“Patients with chronic respiratory diseases should continue their treatment as usual. This also applies if the treatment plan includes corticosteroids. […]. If they contract COVID-19 on top of uncontrolled asthma, the situation will be much more critical than if they continue corticosteroid inhalation while taking careful precautions to avoid becoming infected” states Prof. Dr. Wolfgang Kamin in an interview with PARI.
This makes it all the more important that respiratory patients have a well-managed treatment regimen that they adhere to. Adherence can be significantly affected by usage errors, as both a lack of effect and local side effects can lead to patients discontinuing their therapy of their own accord [7]. Usage errors are greatly reduced when patients use nebulisers for their therapy, as they only require simple, tidal breathing.
Furthermore, secretolysis by inhaling hypertonic saline, which is important for many respiratory patients, can only be achieved by using a nebuliser. Nebulisation is an important component of the treatment of patients with cystic fibrosis, for instance. As Prof. Dr. Rainald Fischer states in an interview with PARI: “Respiratory patients who use a nebuliser should continue to do so.”
Brigitte Schmailzl, physiotherapist for the German bobsleigh team and for the Reference Centre for Respiratory Therapy in Sport talks about how inhalation therapy is an important factor in virus protection for everybody.

Around 34 % of all COVID-19 patients suffer from excessive sputum production [14]. Oscillating Positive Expiratory Pressure (O-PEP) devices can be helpful to facilitate sputum clearance and reduce exhaustion due to coughing, in patients with COVID-19 who have chronic pulmonary disease.[15] It may thus be a physiotherapeutic intervention in hospital-admitted patients with confirmed / or suspected COVID-19.[14]
Some PEP-Systems such as the PARI PEP S can also be combined with the nebulisation of drugs and saline solutions to save valuable time for patients and caregivers. Beside the treatment of COVID-19 patients, PEP therapy allows effective, convenient, and repetitive mobilisation of bronchial mucus for patients suffering from CF, COPD, bronchiectasis or asthma.
[1] Pfeifer M et al.: Position Paper for the State-of-the-Art Application of Respiratory Support in Patients with COVID-19 (https://pubmed.ncbi.nlm.nih.gov/32564028/)
[2] https://www.nice.org.uk/guidance/ng168/resources/covid19-rapid-guideline-communitybased-care-of-patients-with-chronic-obstructive-pulmonary-disease-copd-pdf-66141907467973
[3] Voshaar T et al: Empfehlungen für die Auswahl von Inhalationssystemen zur Medikamentenverabreichung. Pneumologie 2001; 55(12): 579-86
[4] https://www.rki.de/DE/Content/InfAZ/N/Neuartiges_Coronavirus/Steckbrief.html#doc13776792bodyText15 Edwards, D. A. Proc Natl Acad Sci U S A. 2004; vol 101, no 50: 17383 -88
[6] Fink et al: Reducing Aerosol-Related Risk of Transmission in the Era of COVID-19: An Interim Guidance Endorsed by the International Society of Aerosols in Medicine. Journal of Medicine and Pulmonary Drug Delivery, Vo.33, No. 0, 2020
https://www.paediatrische-pneumologie.eu/fileadmin/pdf_Dokumente/2020/Statement_Asthma_und_COVID-19_F.pdf
[7] Rootmensen GN et al: Predictors of incorrect inhalation technique in patients with asthma or COPD: a study using a validated videotaped scoring method. J Aerosol Med Pulm Drug Deliv 2010; 23(5): 323-8
[8] Machado R. et al., Hypertonic saline solution inhibits SARS-CoV-2 in vitro assay. BioRxiv preprint 2020. https://www.biorxiv.org/content/10.1101/2020.08.04.235549v1
[9] Reeves EP et al. Hypertonic saline in treatment of pulmonary disease in cystic fibrosis. The Scientific World Journal 2012; doi:10.1100/2012/465230
[10] Ramalingam S, Graham C, Dove J, Morrice L, Sheikh A. A pilot, open labelled, randomised controlled trial of hypertonic saline nasal irrigation and gargling for the common cold. Sci Rep 2019;9:1015
[11] NCT. Hypertonic Saline Nasal Irrigation and Gargling in Suspected or Confirmed COVID-19 (ELVIS COVID-19). 2020; https://clinicaltrials.gov/ct2/show/NCT04382131
[12] NCT. Hypertonic Saline for COVID-19 Symptoms. 2020; https://clinicaltrials.gov/ct2/show/NCT04465604
[13] https://www.lungenaerzte-im-netz.de/news-archiv/meldung/article/einfaches-inhalieren-kann-troepfcheninfektion-effektiv-eindaemmern/
[14] Thomas P, Baldwin C, Bissett B, et al. Physiotherapy management for COVID-19 in the acute hospital setting. Recommendations to guide clinical practice. J Physiother. 2020;(1).
[15] Yang L-L, Yang T. Pulmonary rehabilitation for patients with coronavirus disease 2019 (COVID-19). Chronic Dis Transl Med. 2020;6(2):79-86.