
More than two years have past since we first became aware of Corona (SARS-CoV-2). There are now vaccines and at the same time the virus has changed again and again. What we know so far: the vaccines continue to provide reliable protection against serious diseases and most infections are now rather mild. Regardless of the severity of disease, those who have recovered are not necessarily well [1, 2, 3]. Many of those affected are still struggling with the long term consequences.
The phenomena, now routinely referred to as Long Covid, is still a mystery to researchers, physicians and those affected alike. You can read here about the symptoms of Long Covid in the airways. Furthermore you can learn what proven treatments can be recommended also for the treatment of Long Covid.
Numerous researchers haven been grappling with this question in recent months. In general, the term Long Covid is used when patients continue to exhibit symptoms weeks and months after recovering from infection with SARS-CoV-2. Those affected are sometimes also referred to as “long-haulers”, that is to say they are carrying (“hauling”) the symptoms around for a long time.
The period of time for which this term applies has yet to be defined precisely. Sometimes the term is used to refer to those still experiencing symptoms 3 weeks after the “post acute” phase, considerably shorter than the 12 weeks of “chronic-Covid-19-Symdrome” (CCS). Physicians often use the term “post-covid-syndrome” and commonly refer to “post-covid treatments”. The term Long Covid, however, has been established as a term for those who continue to present symptoms after resolution of their infection. The use of this term by lay persons in particular on the internet means that is becoming increasingly established [4].
The findings from many observational studies are now available. These confirm: not all persons recovered from Covid-19 are truly well. The results of a recently published meta analysis of 15 studies (only included studies with more than 100 participants) showed that around 80% of those infected with SARS-CoV-2 exhibited one or more long-term symptoms. [5]
A further study in which a total of 2113 persons were questioned showed a similar result. Some of the participants came from two Facebook groups for Coronavirus patients with persistent symptoms in the Netherlands and Belgium. The remainder from a panel of persons who had registered on the website of the Lung Foundation Netherlands. They asked about the presence of 29 different symptoms at the time they were recorded (retrospectively) as well as at the follow-up examination (average ±SD 79 ±17 days after symptoms appeared).
Fatigue, headaches and shortness of breath belonged to the most frequent long-term consequences with a tightness in the chest and coughing also being reported in frequent cases. Noteworthy is furthermore that around 18% of patients were still reporting of having mucus in their lungs even after 79 days (see chart [6]).
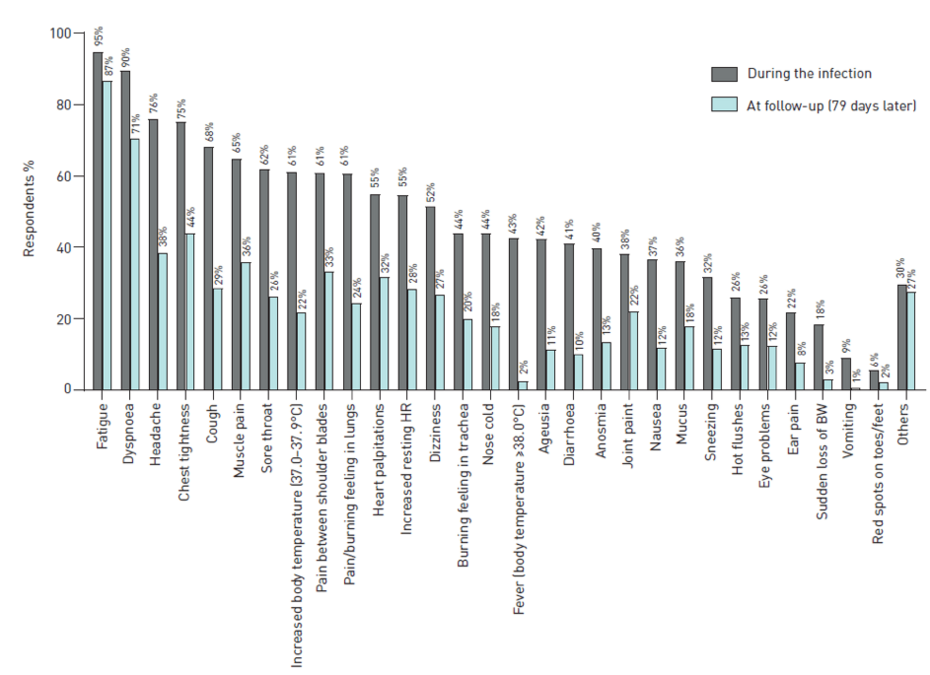
The results from the studies highlight that a considerable portion of patients with an acute SARS-CoV-2 infection suffer with longer term problems of their airways [5, 6]. To date over 110 Million Covid-19 cases have been confirmed (February 27th 2021), meaning that a considerable number of persons are likely to have long-term problems with their lungs. This number will of course vary depending on the incidence of COVID-19 in different countries.
Prof Rohde, head of the post-Covid ward, pulmonology and allergology at the University Hospital in Frankfurt, also reported seeing Long Covid patients with a hyper responsive bronchial system and shortness of breath: “Three different patterns can be recognised. One is the so-called hypersensitivity of the airways. That means that coughing can result relatively quickly from certain stimuli such as for example cold air or exertion. The second is the development of a real shortness of breath meaning that any exertion leaves them not only tired and exhausted but are out of breath much faster. This is often on account of structure changes to the tissue in their lungs” [7]. Some of these patients are already receiving treatment. Another group will likely soon contact their GPs or ask themselves how they can best deal with such long-terms problems of their airways.
The good news is that coughing and bronchial hyperresponsiveness can be treated well by nebulising saline solution. In the case of cough, a differentiation should be made between productive (with mucus) and dry coughing (without mucus). Whilst a dry cough is best treated with isotonic saline (saline content = 0,9%), hypertonic saline (saline content = 3-7%) is recommend to help mobile mucus. [8]
Saline solutions can be inhaled with a compressor or a mesh nebuliser system. Decisive for an effective inhalation is the volume of aerosol droplets small enough to be able to reach the lungs (≤ 5µm). The higher the amount of droplets under 5µm, the better the deposition in the lungs. Decisive is furthermore how many of the droplets are able to reach the lungs in a certain time period. The “Respirable Drug Delivery Rate” (RDDR) is calculated based on both these values. The higher the RDDR, the more efficient the nebuliser. The more efficient the nebuliser, the shorter the inhalation time and as a consequence the higher the acceptance of the therapy amongst patients. The RDDR thus is an important factor when evaluating the quality of an inhalation system.
PEP Therapy can play an important part in the management of COVID-19 patients. This technique of cleaning the airways, thus reducing the ill effects and a potentially lessening a progressive worsening of symptoms [9, 10]. Also patients with “Long Covid” symptoms associated with problems of the airways (build up of mucus in the airways) could profit from it.
Dr Thomas Voshaar, Head Physician at the Bethanien Pulmonology Hospital in Moers and medical advisor of the German Heath Ministry throughout the Covid-19 pandemic made the following statement on PEP therapy to treat Covid-19 patients: “in particular PEP therapy was a part of the management of the Covid-19 infection. Since similar to CPAP, the active use of a PEP system helps improve gas exchange, avoid or reopen microatelectases and mobilise secretions to promote secretolysis“ (https://www.pari.com/int/pari-physician-portal/news/covid-19-therapy-from-an-aerosol-experts-perspective/).

The PARI PEP S system can be combined with nebuliser therapy. This saves time which can markedly increase the adherence by patients.
PARI BOY Classic is a powerful nebuliser system with an above average efficacy (measured according to RDDR). PARI BOY Classic can be used with the PARI PEP S system thus enabling a time-saving combination of inhalation and PEP therapy.
Which inhalation solution shall be used is determined by the kind of cough the patient experiences: For the treatment of dry cough with hyper responsive bronchial system an isotonic saline such as PARI Inhalation Solution 0,9% would be a good choice.
If the patient experiences a productive cough (with mucus) a hypertonic saline such as PARI MucoClear 3 % should be used for the inhalation treatment.
[1] Greenhalgh T, Knight M, A’Court C, Buxton M, Husain L. Management of post-acute covid-19 in primary care. BMJ 2020;370:m3026
[2] Townsend L, Dowds J, O’Brien K, Sheill G, Dyer AH, O’Kelly B, u. a. Persistent Poor Health Post-COVID-19 Is Not Associated with Respiratory Complications or Initial Disease Severity. Ann Am Thorac Soc. 8. Januar 2021;AnnalsATS.202009-1175OC.
[3] Davis HE, Assaf GS, McCorkell L, Wei H, Low RJ, Re’em Y, u. a. Characterizing Long COVID in an International Cohort: 7 Months of Symptoms and Their Impact [Internet]. Infectious Diseases (except HIV/AIDS); 2020 Dez [zitiert 12. Februar 2021]. Verfügbar unter: http://medrxiv.org/lookup/doi/10.1101/2020.12.24.20248802
[4] Mahase E. Covid-19: What do we know about “long covid”? BMJ. 14. Juli 2020;m2815.
[5] Lopez-Leon S, Wegman-Ostrosky T, Perelman C, Sepulveda R, Rebolledo PA, Cuapio A, u. a. More than 50 Long-term effects of COVID-19: a systematic review and meta-analysis. :22.
[6] Goërtz YMJ, Van Herck M, Delbressine JM, Vaes AW, Meys R, Machado FVC, u. a. Persistent symptoms 3 months after a SARS-CoV-2 infection: the post-COVID-19 syndrome? ERJ Open Res. Oktober 2020;6(4):00542–2020.
[7] Folge 67 des NDR-Corona Updates (Drosten / Ciesek, Minute 5:30 https://www.ndr.de/nachrichten/info/67-Coronavirus-Update-Der-lange-Schatten-des-Virus,podcastcoronavirus268.html
[8] Kardos P, Dinh Q, Fuchs K-H, Gillissen A, Klimek L, Koehler M, u. a. Leitlinie der Deutschen Gesellschaft für Pneumologie und Beatmungsmedizin zur Diagnostik und Therapie von erwachsenen Patienten mit Husten. Pneumologie. März 2019;73(03):143–80.
[9] Thomas P, Baldwin C, Bissett B, Boden I, Gosselink R, Granger CL, u. a. Physiotherapy management for COVID-19 in the acute hospital setting. Recommendations to guide clinical practice. J Physiother. 23. März 2020;(1).
[10] Hellmuth T, Hoppe D, Teschler S, Hoheisel R, Hillmann T. Empfehlungen der Deutschen Gesellschaft für Pneumologie und Beatmungsmedizin e. V. (zu Hygienemaßnahmen bei der Behandlung von PatientInnen mit Lungenerkrankungen in der ambulanten Physiotherapiepraxis in Zeiten der SARS-CoV-2-Pandemie. Dtsch Ges Für Pneumol Beatm E V DGP. 3. November 2020;
You have questions, suggestions or would like to talk to us about scientific findings?
Global Senior Medical Advisor
+49 (0) 8151 279 5 213