People with a chronic lung disease often experience respiratory distress. PEP therapy can help alleviate this. Marlies Ziegler, a physiotherapist, explains how and why PEP therapy works.
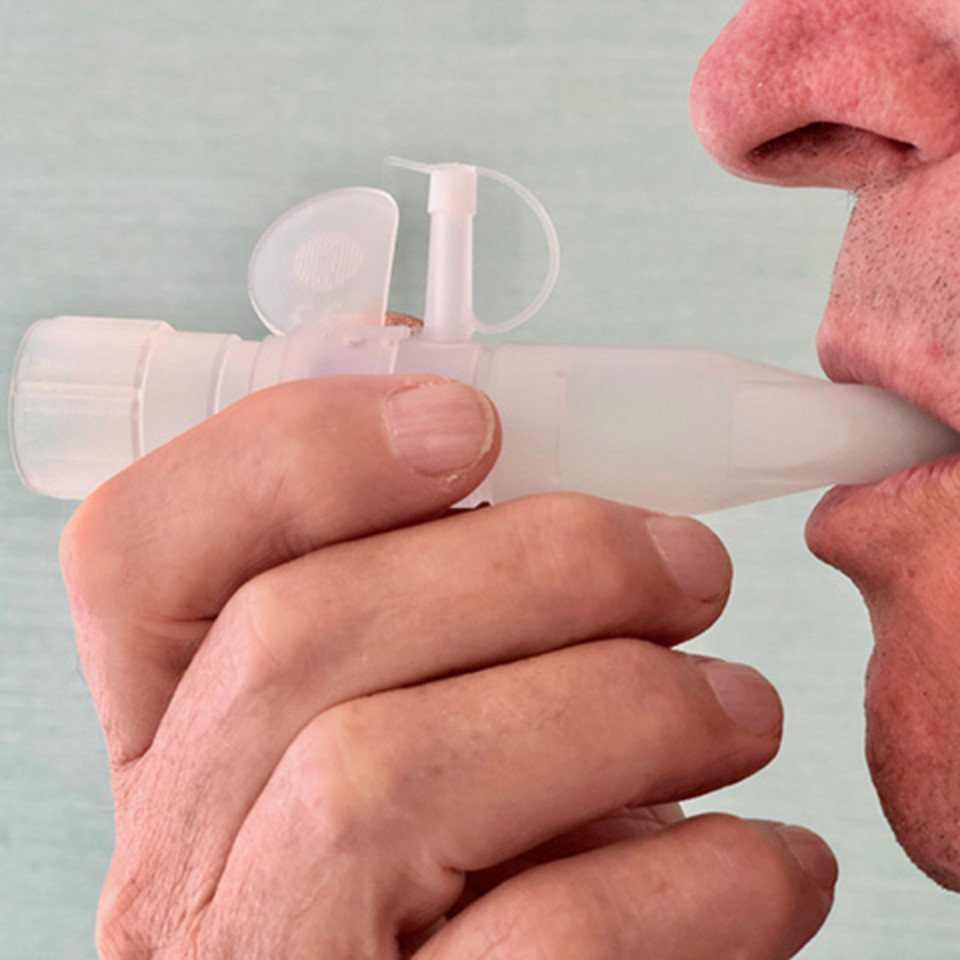
People with a chronic lung disease such as asthma, COPD, cystic fibrosis (CF) or primary ciliary dyskinesia (PCD) often experience respiratory distress. PEP therapy can help alleviate this. We have teamed up with Marlies Ziegler, a physiotherapist, to explain how and why PEP therapy works.
PEP breathing means: exhaling against positive pressure or resistance. “PEP therapy refers to various breathing techniques and respiratory aids which patients can use to exhale against a resistor. A resistor is a form of external resistance that stabilises the bronchial tubes when the patient exhales”, explains the physiotherapist Marlies Ziegler.

“It is important to remember: PEP therapy cannot ‘cure’ shortness of breath, hyperinflation of the lungs, chronic build-up of mucus or unstable airways. Regular use does, however, reduce symptoms and may limit any potential escalation of symptoms.”
Marlies Ziegler
Physiotherapist from Munich
PEP therapy keeps the pressure in the bronchial tubes constant. This prevents the bronchial tubes from collapsing, or at least slows down this process, allowing them to remain open until the end of the exhalation. This makes it easier to exhale, and patients can exhale for longer than they can without resistance or PEP.
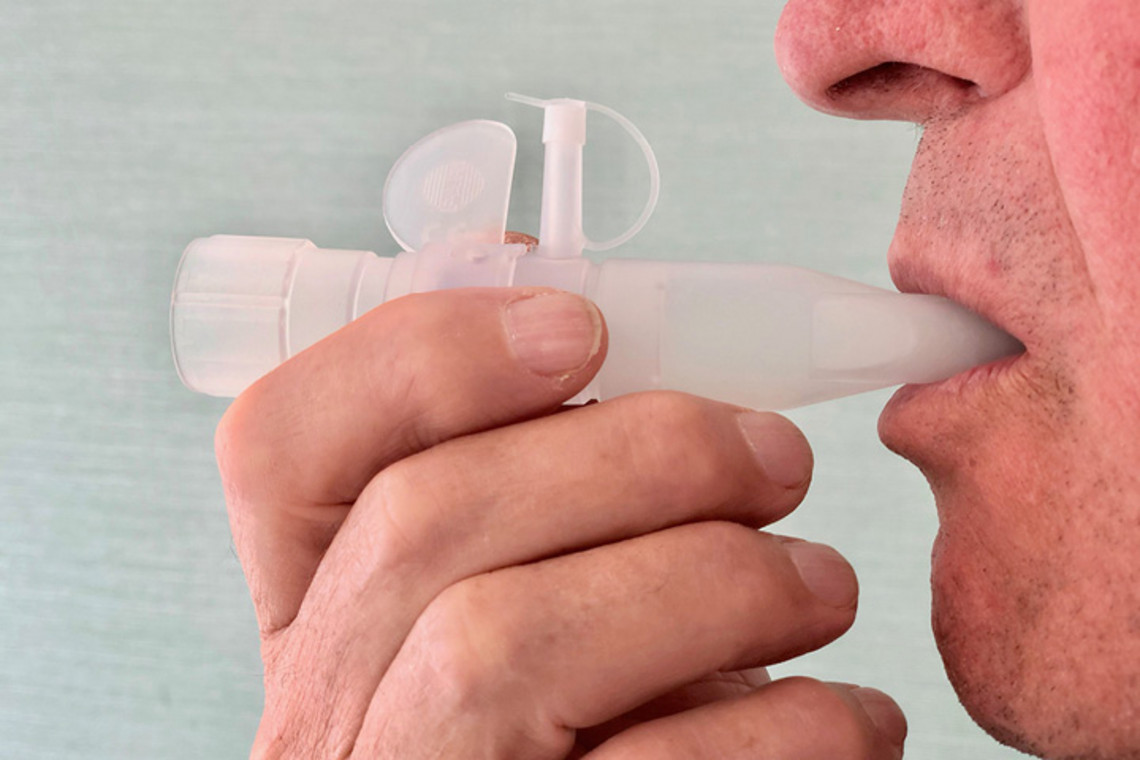
The physiotherapist gives her patients the following tip: “If you feel the urge to cough when you are performing PEP therapy, for instance if mucus is loosened and causing tickling in your bronchial tubes, simply cough into the PEP. If the lungs are damaged, coughing can destabilise the bronchial system. The pressure that builds up from outside during a cough from the muscles and that is therefore exerted on the chest is too high. The bronchial tubes may collapse. If you cough into the PEP system, the flow is slowed down, there is a more even drop in pressure, the bronchial tubes remain more stable and it is easier to empty the lungs despite the cough.”
PEP therapy can be successfully combined with mobilisation exercises for the chest and positioning to increase effectiveness.
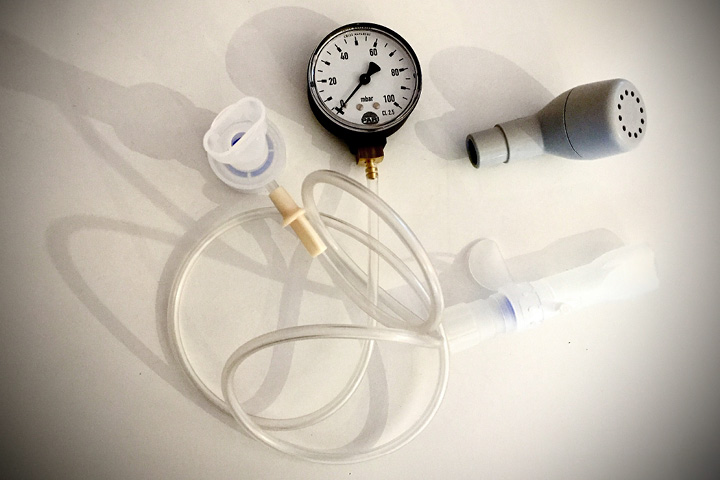

Controlled exhalation can be divided into patient-controlled and device-controlled (respiratory aid) resistance.
Examples of patient-controlled resistance are:
Examples of device-controlled resistance are:
Ask your physiotherapist in an individual consultation which is the best type of straw to use.
All PARI PEP systems and nebulisers can be prescribed by doctors as needed. But the systems are also available through pharmacies, online pharmacies, and large online shops.
Marlies Ziegler works as a physiotherapist in a private practice in Munich. She specialises in respiratory physiotherapy. She has been treating patients with chronic obstructive and restrictive airway diseases such as asthma, COPD, cystic fibrosis (CF) and primary ciliary dyskinesia (PCD) for 20 years.
Note: The information in this blog post is not a treatment recommendation. The needs of patients vary greatly from person to person. The treatment approaches presented should be viewed only as examples. PARI recommends that patients always consult with their physician or physiotherapist first.