Inhalation has an important role to play in people who have a tracheostomy. Here are some practical tips on inhalation therapy and breathing freely.
Inhalation has an important role to play in people who have a tracheostomy. Here are some practical tips on inhalation therapy, breathing freely and FAQs from patients with a tracheostomy.
Once a tracheostomy tube has been placed, as well as speech therapy support, secretion management is an essential part of the treatment. Inhalation therapy is a standard procedure in delivering this therapy.
Jürgen Lippert knows all about this from his own, first-hand experience. The Vice President of the German Federal Association of Larynx Surgery Patients, is living with a tracheostomy. He also inhaled NaCl (= saline solution) after his surgery. After surgery, patients have to learn how to breath properly through the tube, how to speak and how to clear mucus. If the mucus is liquid and loosened, this is easier to do.
Inhalation therapy is not recommended immediately after surgery, but in general. Tracheostomy patients have to keep their tracheostomy tube clean and clear at all times by removing any secretions. Inhalation helps them do this, as it liquifies the secretions and helps prevent them from drying. This makes the mucus easier to cough up.
The role inhalation plays in their therapy varies from person to person and doctors adapt the therapy to meet the patient’s individual needs.
Inhalation therapy with nebulisers like the PARI LC SPRINT Tracheo helps liquify the secretions in the airways. This makes it easier to cough up or suction away the mucus from the tracheostomy tube and improves the gas exchange in the lungs. This is because excess mucus can block the bronchial tubes. This, in turn, can affect breathing or the gas exchange. A clean tracheostomy tube improves breathing and prevents infections.
Generally, patients with a tracheostomy inhale NaCl 0,9 % (= isotonic saline solution). If the patient has problems with a large amount of mucus in the airways or very viscous mucus, it may help to inhale hypertonic saline solution such as MucoClear 3% or MucoClear 6%. Inhalation can also support the targeted release of medication in the lower airways.
Inhalation therapy in patients with a tracheostomy can bring relief in various situations, such as:
It may make sense to use the inhalation therapy more often in autumn and winter. This is because central heating indoors dries out the mucous membranes. Inhalation with isotonic saline solution helps prevent this from happening, by keeping the airways moist. Moist mucous membranes are better positioned to fight off pathogens.
In autumn and winter there are more viruses doing the rounds than usual. Even a mild infection can result in thicker mucus and more respiratory problems. In this case too, more frequent inhalation therapy makes sense to keep the tracheostomy as clean as possible and so prevent an infection in the lower airways.
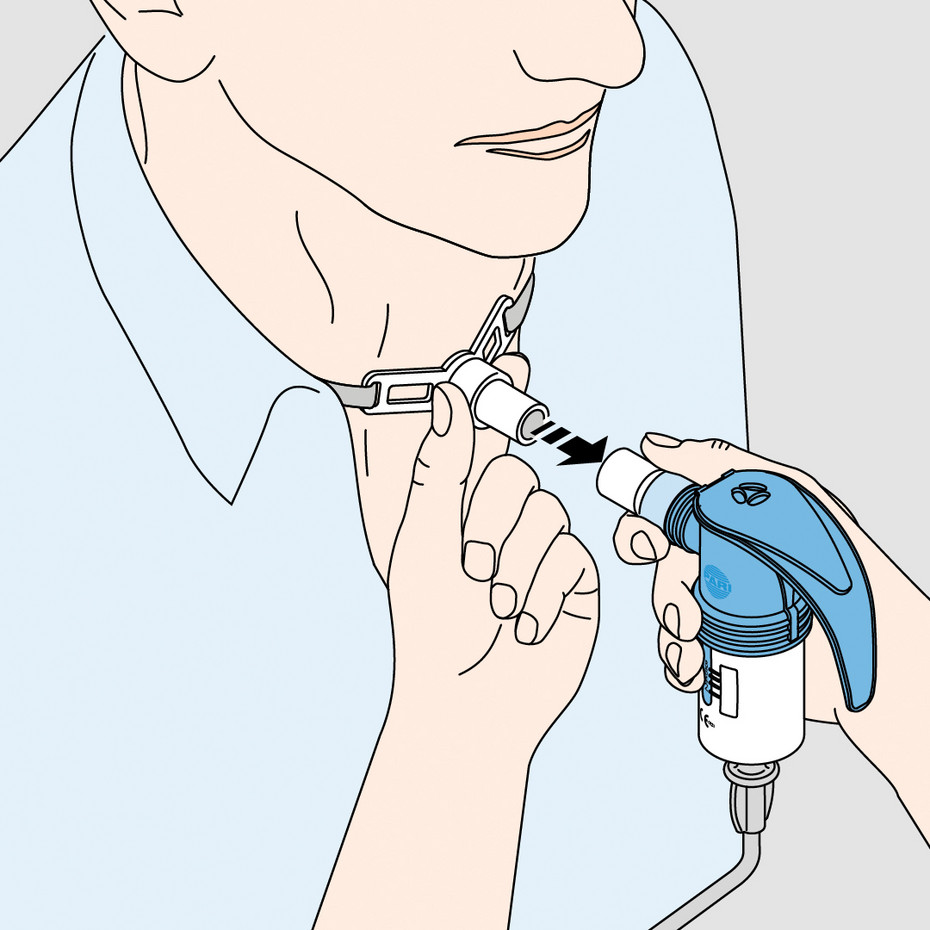
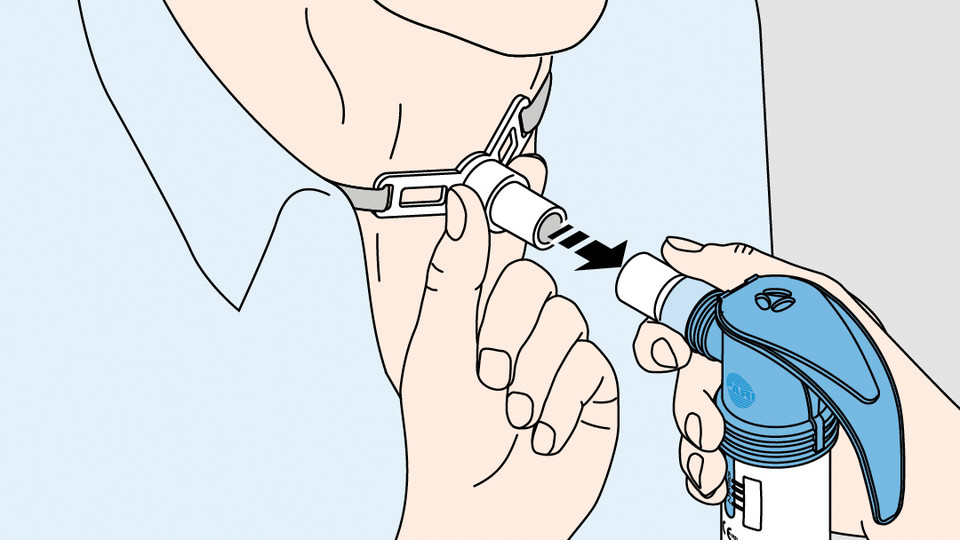
You can use nebulisers with masks or adapters especially designed for inhalation with a tracheostomy. You can precision fit these to the tracheostomy on your neck. This ensures efficient and effective inhalation therapy. PARI has nebulisers designed especially for children and adults with a tracheostomy.
The set includes the nozzle nebuliser (orange nozzle attachment) with valve system, the PARI Tracheo mask adapter, and also the PARI tracheostomy mask and a connection tube with adapter. The mask is especially soft and is fitted tightly over the tracheostomy.
The nozzle nebuliser (orange nozzle attachment) with valve system with the LC Tracheo adapter is fitted directly over the tracheostomy and provides a perfect, snug fit. A connection tube with adapter is also included in the set.
Both nebulisers are compatible with all PARI compressor inhalation devices such as the PARI BOY or the PARI COMPACT2.
For home use, clean the nebuliser after each use and disinfect once a week to prevent bacterial growth. To do this, disassemble the nebuliser into its individual parts and clean with clear water. Then boil the parts in a pot or put them in a steriliser for baby bottles.
Ask your doctor for advice on how often to use the inhalation therapy and which solution to inhale. Many patients with a tracheostomy inhale two to four times a day with isotonic NaCl solution (0.9% salt content). A hypertonic saline solution may make sense if there is a large amount of mucus.
PARI inhalation devices provide fast and efficient inhalation therapy. This is why inhalation therapy with a nebuliser from PARI generally takes 4 to 5 minutes (for 2.5 ml volume of solution with the PARI BOY).
Note: The information in this blog post is not a treatment recommendation. The needs of patients vary greatly from person to person. The treatment approaches presented should be viewed only as examples. PARI recommends that patients always consult with their physician or physiotherapist first.