A trip to Australia with a camper van entails risks for a cystic fibrosis patient. Even so, the PARI blog author, Alex, risked the trip and describes the challenges, the tour and her unforgettable experiences.

A trip to Australia would no doubt be special for anyone, but for me, the trip “Down Under” was both a dream journey and a potential risk, because I have cystic fibrosis (CF). It is a genetic disorder that is destroying my lungs bit by bit. A long journey which involves, at a minimum, a 23-hour flight might be too much for my lungs to handle. But in the winter of 2017 I drove along the Australian east coast in a camper van for three weeks anyway. It was the most wonderful trip of my life.
When healthy people want to drive a camper van around Australia, they just do it. Maybe they have to save up for a while, but this financial hurdle is probably the only thing that stands in their way. For me, a trip to Australia presents multiple challenges, because I have CF.
CF is a genetic disease in which the secretions from many of the body’s glands are more viscous than those of healthy people. This viscous mucus plugs up vital organs, primarily the lungs. The excessive mucus is an ideal breeding ground for bacteria, making me very susceptible to infections and lung inflammation, which in turn lead to the destruction of my lung tissue. To delay this destructive process as much as I possibly can, I perform a special CF nebuliser/respiratory therapy twice a day for an hour and take many drugs. Despite all these efforts, my pulmonary function and capacity will continue to deteriorate in the future. At some point I will no longer be healthy enough to go on long-haul flights. Even now there is some risk a 23-hour flight and an intensive trip might be too taxing for my lungs. But my health won’t get better, which is why it’s now or never – I’m off to Australia with my husband and child!
In addition to the usual travel preparations everyone is familiar with, I need to do extra research and make additional arrangements for my CF. Along with my regular medications, I also need to get emergency medications and a certificate from my doctor about bringing my cocktail of drugs with me.
Key questions need to be answered: Where are CF clinics located in case I have an emergency? Where can I go if my nebuliser stops working? Which campsite offers the ideal hygienic conditions to avoid infection-causing germs? Where can I find distilled water which I need to sterilise the nebuliser head of my device. However, the most important task is packing my medications and accessories for my nebuliser and respiratory therapy. Everything is packed in my carry-on because if anything gets lost, it will be a very big problem.
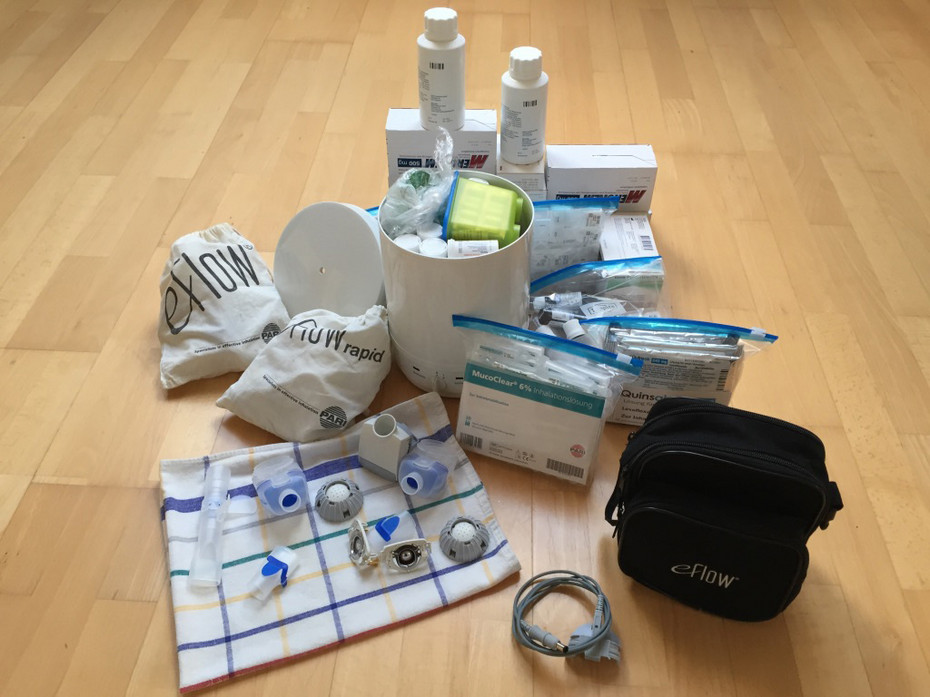
Per day, I take more than 35 pills and perform nebuliser therapy twice a day with at least five different medications. For a three-week trip that’s quite a pile, consisting of approximately 800 tablets, 300 ampoules of solution for inhalation, such as isotonic and hypertonic saline solution, and several metered dose inhalers. Unsurprisingly, it took me a good 4 hours to pack all my treatment stuff: Finding and counting out medications, counting again to be sure, repacking so they take up as little space in my carry-on as possible, cleaning, sterilising, air drying, and packing all nebuliser heads and respiratory therapy devices. For the 3-week Australia trip, I had so much medical equipment that I had to put some in my husband’s carry-on and some in my child’s. I also had to keep in mind that I had to perform therapy and take my medications twice during the 23-hour trip! So, I stored my nebuliser accessories and medications in a separate bag so I could access them easily.

Going through my nebuliser and respiratory therapy is a very intimate process. I only do it in front of my family and very close friends, and the thought of having to do it sitting on a plane between people I didn’t know was horrifying. Sometimes I have to cough a lot, and the mucus rattles in my airways. Not everyone needs to witness that, but on a 23-hour flight I had no other choice. So, I put a large towel over my head, turned my nebuliser device on and started. I don’t know if it was because of the towel, which acted as a misting tent, or if it had something to do with the atmosphere in the airplane, but the hypertonic saline solution tasted much saltier than usual, but it was kind of nice. I was already aware of the benefits of my eFlow®rapid, but I’ve never been so grateful because it’s practically silent, nebulises the medication within 5 minutes and can be battery-operated meaning I could use it on board. I must admit though that I only did my therapy for 20 minutes instead of the usual 60 minutes.
We were on the road almost every day. Luckily my husband did all the driving on our holiday. He called himself my chauffeur. But this way I was able to use our time for therapy. For the first time in my life I didn’t have to get up an hour-and-a-half earlier than the rest of the family to take care of my therapy before the “normal” day started. My husband started the engine, I put batteries into the eFlow and off we went.

On the days when we didn’t drive anywhere, I used my nebuliser outside the camper van – of course only when the rest of the campground was still asleep. I did neglect my stretching and mobilisation exercises during our holiday though because it was too cramped in the camper, and I didn’t have the time with our packed travel itinerary. Instead, I used the PEP S System, a compact respiratory therapy device for secretion mobilisation, more often during the drive. Storing my medications was also not without its complications - outdoor temperatures were up to 34°C, and the camper became extremely hot when we left it for outings. Many medications should not be stored over 25°C because they go bad. So I stored the majority of them in the camper van’s refrigerator. Unfortunately, there wasn’t much room left in there for food.

To be honest, I don’t like camping too much because I have to use public toilets and showers which tend to have worse hygienic conditions than your bathroom at home, i.e. more viruses and bacteria. In particular, the microbe Pseudomonas aeruginosa, which thrives in moist environments, is a problem for people with CF. For example, it’s swirled into the air when a toilet is flushed with the lid up. Some campground toilets don’t even have lids. Pseudomonas can colonise the lungs of CF patients, causing terrible inflammation. One reason we chose to get a camper van was so we could have our own toilet and shower. What I hadn’t thought about before starting the trip was that Pseudomonas can develop in the camper van’s water tank. This was problematic in several ways. Better not to shower, wash my face or brush my teeth with the water from the tank. So I ended up using the bathrooms at the campgrounds anyway. Incidentally, the water was treated with chlorine. When washing the dishes, rinsing vegetables and fruit with the tank water I had a bad feeling that I was still at risk of ingesting Pseudomonas. So, I almost exclusively used water that we bought at supermarkets. When it became clear that driving around with aa toilet that isn’t emptied daily is rather unappetizing when it’s 34°C outside, we occasionally freedom camped. I was so glad to have my broad-spectrum antibiotic with me.
Australia’s east coast is definitely a suitable travel destination for CF patients – apart from the inhumanely long flight. The sea air, the warm climate and low smog levels are ideal for people with lung problems. In addition, Australia has strict anti-smoking laws. All hotels, hostels, restaurants, cafés and pubs etc. are 100% non-smoking. Smoking is even banned from outside areas, such as pub terraces and gardens, and from entrances. Something I noticed right away was that in Australia, people smoke less than for example in Germany. Over our 3-week holiday I saw only 20 smokers – yes, I actually counted! I met most of them in Sydney and Melbourne - the handful I met on the coast were mostly (German) tourists.
Alex (pseudonym), who was born in 1977, has cystic fibrosis. She is a freelance editor and has one child. She writes personal stories for the PARI blog about living with cystic fibrosis and the challenges associated with the disease, and she gathers practical tips on the topics of breathing and nebuliser therapy.
Note: The statements made in the report are the individual view of the person reporting. They do not necessarily reflect the PARI view or the general state of science.