Life changes radically with a donor lung – overwhelmingly for the better. But there are dark sides as well. In this interview, Reiner Heske details what life is like after a lung transplant.

Reiner Heske lives with cystic fibrosis (CF). This hereditary disease destroyed his lungs over time, so he received a donor lung in 2013. After the transplantation his life changed radically – overwhelmingly for the better. While a transplanted organ gives a new lease on life, there are down sides too. In this interview, Reiner Heske shares his experiences post-op and with a donor lung.
Reiner Heske: Lung transplantation is a pretty violent procedure, during which your ribcage is cut open and your ribs are forced apart. My operation took six hours. First one lung, then the other was replaced. In my case my lungs were actually so adhered that they weren’t able to be removed easily, and had to be cut out. This caused severe post-op bleeding. After the operation I also needed several units of blood products and blood plasma because I was on the verge of losing consciousness several times.
Reiner Heske: First of all, I was really glad to be alive. Waking up was quite joyous because to my surprise a very nice cystic fibrosis doctor I knew from before and was now apparently working at the transplantation clinic was there to greet me. I hadn’t seen her in years. That was a nice coincidence. In the recovery room my mind was still pretty fuzzy from the anaesthesia, but physically I was doing relatively well. The tube for the ventilator was in my throat, but I wanted to be able to talk again as soon as possible. You can’t do with a tube down your throat. So I wrote short messages on pieces of paper to communicate. Fortunately the tube could be removed quickly. In the recovery room an ultrasound was done of the places or incisions where the donated lung had been sutured to my trachea. Post-op I was in hospital for three weeks, some of that time in intensive care. It was actually a pretty stressful time. I shared a room with two other patients. Sleeping was out of the question during this time because we were all connected to monitors that beeped non-stop.
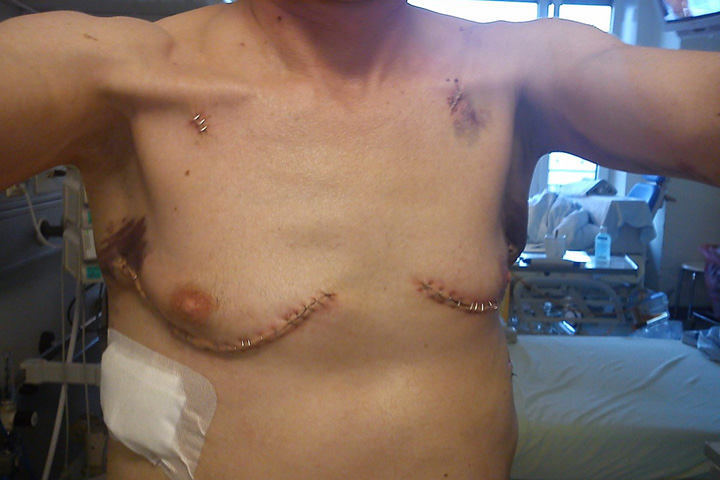
Reiner Heske: Actually not at first. It felt like I wasn’t able to fill my lungs with air directly. Inhaling in particular was very hard in the beginning as if I had a tension belt around my ribcage that was hindering my breathing movements. My ribcage hurt and I didn’t dare that I could inhale past this obstacle. It felt like my ribcage would be torn apart if I were to take a deep breath. As a result of having a severe lung disease for decades, I had developed a very rigid and pronounced barrel chest. This is why my ribcage was so inflexible. My inflexible ribcage was now pressing against lungs that were in great shape. My ribcage was used to my old lungs with their very low lung volume of around 0.9 litres FEV1. With my donor lungs I can produce 3.7 litres on the FEV1. This is an improvement of more than 300 per cent. My body had to adjust first and get used to my donated lungs’ capacity – apparently painfully initially. Post-op, I also had drains on the right and left sides of my ribcage so wound secretions could drain out. They didn’t exactly improve my quality of life.
Reiner Heske: After the transplantation, I was on oxygen for two or three days. To be honest, I was anxious about the moment when the tube would be removed from my nose. After all, that tube had been a part of my life for years and had ensured my survival. I was connected to an oximeter and could see that my saturation was 94 to 95 per cent even without supplemental oxygen. Fantastic. I was bowled over. Because my donor lungs were not even fully expanded yet, meaning that the saturation levels would go up even more in the medium run. I was not able to breathe normally and unhindered until three to four weeks after the transplantation. I had the feeling of having a constricted ribcage when inhaling for at least another one to one-and-a-half hears. I think it is a safe assumption that exercise helped me overcome this feeling of a constricted ribcage relatively quickly.
Reiner Heske: I used a variety of breathing aids. This included devices I could use to exercise and strengthen my breathing. I also had the PARI PEP system, which I was already familiar with from my CF therapy. At first, wound secretions were still found my lungs. For example, the donor’s mucous membranes detached. My lungs formed a new mucous membrane over them. To help mobilise these clumped, old mucous membranes and the secretions, I inhaled table salt twice daily and I used the PEP systems. I also had to inhale an antifungal drug to prevent fungal colonisation in my lungs. In the first weeks after the transplantation I also had a lot of bronchoscopy procedures, repeatedly checking up on the right one and clearing wound secretions from the lungs.
Reiner Heske: This is true. Before the transplantation a day didn’t go by when I was able to leave the house or go to bed without doing inhalation therapy. Now I don’t need to inhale any more for my lungs. I get up in the morning, eat breakfast and go for a run or hop on my bike. The improvement in my quality of life is indescribable.

Rainer Heske: I feel like I have a brand new body. I no longer have shortness of breath, and I have stamina. Right after the rehabilitation phase, I started to do sports and I quickly noticed that I enjoyed exercise. I walked 500 kilometres in the year I had the transplantation. Then in January 2014 I started interval running – alternating running and walking. In April 2014, I completed a 10K run with 30 other racers to raise awareness about organ donation and cystic fibrosis. After that run I felt like king of the world. I suddenly was having so much fun racing against healthy people. To this day it’s hard for me to put this feeling of elation into words.
But cured? No, I am not cured. Transplantation is a treatment, not a cure. I still have the disease. Of course I no longer have the classical cystic fibrosis lung symptoms, but the rest of my body still has the disease. For example, I still have to take enzymes when I eat and continue to have problems with my intestines. It is also still a challenge for my to maintain my weight, especially when I am exercising a lot. This is a problem many people with CF experience. I also have the feeling that my cystic fibrosis is starting to affect other areas. Earlier, I didn’t have any problems with my sinuses. But now I often notice my sinuses are having issues.
Reiner Heske: Mucous accumulates in my sinuses, which makes it hard for me to breathe. Dried mucus forms, which also bother me. There is also the danger that the bacterium Pseudomonas aeruginosa will spread in nasal mucus. So I irrigate my nose daily with a nasal shower. Following a four-weeks-on, four-weeks off schedule, I do inhalation of antibiotics with the PARI Sinus for the nose, to keep reduce the number of bacteria. My current nasal inhalation therapy takes much less time than the inhalation therapy for my lungs before the transplantation.
Reiner Heske: True, many problems were solved. As I said, my lung symptoms are gone. I no longer have shortness of breath, I am fully capable and have been able to complete marathons and bike races up to 120 km long in the past few years. That would have been unimaginable before the transplantation. Then, just walking a few metres pushed me to the limits of my exercise capacity and that was with oxygen therapy. Another positive effect is that my immunosuppressant therapy has almost completely eliminated the allergy-triggered asthma that used to be very bad. There is no comparison between my breathing now and then. My bronchial tubes were always constricted. It was like I was breathing through a straw and it got worse and worse. Breathing was work for me, even when I was young. When I was a child I tried to keep up with my friends, but I was always held back by shortness of breath and by getting infections. My lungs no longer hold me back. Another big difference relates to respiratory infections. For one, in past years I had a lot fewer infections. For another, being sick was associated with much less suffering than before. Before the transplantation, infections were accompanied by unbearable shortness of breath. I had to deal with minutes-long severe coughing fits until tears were running down my cheeks because of the strain. When I got infections, I usually ended up in hospital for several weeks with intravenous antibiotic therapy. Now when I get sick I have a bit of a runny nose or a mild cough. But that’s it – from the perspective of a person with CF that doesn’t count as being sick, it’s so minor.
Of course there are some limitations. For example, it is is hard to build muscle while on cortisone therapy. Another limitation is that I am not supposed to eat raw meat. In general, I have to try to eat foods that are as germ-free as possible. That means ideally boiling, poaching or heating foods so any bacteria and viruses are killed. I also always have to be really strict about hygiene. But I happily accept these limitations. After transplantation the limitations and stresses shift from the body to the psyche.
Reiner Heske: Before the transplantation I tried to do everything I wanted to do. That included participating in public life. I try to do this now too, but since the transplantation I have to pay more attention to hygiene. Because I am taking immunosuppressants I get infections more easily. This is problematic because if I get an infection my immune system might not be able to tell what it should fight. Are they viruses that don’t belong in the lungs or is it the lung itself that doesn’t belong? This is why every infection can promote a rejection reaction. With the corona pandemic my concerns have therefore not gone away, especially since I have already been doing the recommended hygienic practices for years, usually wear a mask and isolate as much as possible. Furthermore, I always have in the back of my mind that every donated organ is rejected at some point. For longs on average it takes ten years. My transplantation was seven years ago. So I can’t help but worry. But statistics are relative.

Reiner Heske: Deterioration of lung function can be an initial sign of rejection of a donor lung. This is why I check my lung function every day at home so I don’t miss anything. There are therapies with which one can at most slow down the rejection. When they don’t work, retransplantation, in other words a second transplantation, is theoretically possible.
Reiner Heske: A second transplantation can only be performed under very specific circumstances. In addition to medical requirements, it depends on the regulations in the country in question. In Germany, for example, cystic fibrosis patients can get a transplantation only up to the age of 60. In addition, all of the parameters have to match and the patient cannot have a history of any malignancies. I only have half my pancreas, gallbladder, appendix, duodenum and parts of my intestine have been removed. I am also over 50 years old. These are the types of thoughts that swirl around in my head. And therefore I could imagine that because of my age alone, the chance of a second transplantation would be slim.
Reiner Heske: I look at it this way: With the donated lungs I have been given the gift of seven years of life that is easy-going, free, and beautiful. So I am very grateful to the donor and their family. For me the step of transplantation was and is the absolute right thing to do. I would advise anyone with a lust for life to risk this step. Of course there are risks involved, of course there are disadvantages, which are presented with no punches pulled during the informed consent discussion. But when is faced with a decision for or against transplantation, usually one does not really have a choice. What would you have to lose? I would do it all over again.
Reiner Heske was born in 1969 with cystic fibrosis, a hereditary disease, and given a lung transplant in 2013. After his transplant, he became physically active and took part in sporting events to raise awareness about cystic fibrosis and the importance of organ donation. He takes part in sponsored runs raise money for cystic fibrosis. In addition to this activism, he also personally organises fundraising runs for cystic fibrosis.
Note: The statements made in the interview are the individual views of the interviewee. They do not necessarily reflect the PARI view or the general state of science.